CLARKSDALE, Miss. -- The first hurdle was getting on the bus. Seventy-four year old Linda Busby hesitated outside a community center where older people were loading up to go get the coronavirus vaccine.
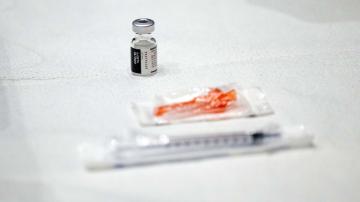
“I was scared, I’m not afraid to say that,” she said Wednesday after getting her shot of the Johnson & Johnson vaccine after encouragement from a staff member and her brother. “I thought I wasn’t going to get it at first. Nobody likes getting shots.”
Busby's hesitance is just what the Biden administration and its allies in the states are combating, one person at a time, as the White House steps up appeals to seniors to get inoculated. The vaccination rate for this top-priority group is reaching a plateau even as supplies have expanded.
About 76% of Americans aged 65 and older have received at least one shot of the COVID-19 vaccines since authorization in December, according to the Centers for Disease Control and Prevention. But the rate of new vaccinations among the group most vulnerable to adverse virus outcomes has dramatically slowed.
It’s a growing source of concern, not only because of the potential for preventable deaths and serious illness among seniors in coming months but also for what it could portend for America's broader population.
“I want to make a direct appeal to our seniors and everyone who cares about them," President Joe Biden said Tuesday, citing “incredible progress” but declaring it's still not enough.
“It’s simple: Seniors, it’s time for you to get vaccinated now. Get vaccinated now.”
By government estimates, about 12.9 million American seniors have yet to receive their first shot. Even though they were the first age group prioritized for shots, more than 23% of those 75 and older have yet to be vaccinated.
Supply constraints initially slowed the pace of senior vaccinations, but not for months for those in high-priority age groups. Instead, officials say, the slowdown is caused by a mix of issues, from people having difficulty finding and getting to inoculation sites to vaccine hesitancy.
Closing the gap will require taking into account all the obstacles for seniors, be they technological, transportation or personal hesitance, said Sandy Markwood, CEO of the National Association of Area Agencies on Aging, who acknowledged the vaccination rates 'for older adults has somewhat plateaued.”
It’s a potential harbinger of the challenges to come with other demographic groups. All adult Americans will become eligible for vaccination in the next two weeks, although the process of administering enough shots to begin returning to “normal” will take months longer. Many states, even as they throw open the doors on eligibility, are still maintaining priority vaccination systems, or dedicated distribution channels, to keep seniors who want the vaccine at the front of the line.
Dr. Anthony Fauci, the nation’s top infectious disease expert, has predicted that between 75% and 85% of the population may need to be vaccinated to reach “herd immunity” and bring an end to the outbreak in the U.S.
That’s one reason the White House and states have moved to step up assistance programs for seniors and public education campaigns.
Markwood credited the administration’s $1.9 trillion rescue plan for providing funding necessary “to go out there and do that more intensive, sometimes one-on-one outreach” with seniors, saying, “It’s that last mile, the last group who need the extra support, that’s going to take that extra outreach and time."
Even more help is on the way.
Beginning next week, the administration is launching a $100 million effort to fund community organizations providing “high-intensity” support to at-risk seniors and those with disabilities through the Department of Health and Human Services. That includes assistance with booking appointments, traveling to vaccination sites and other support through the vaccination process.
Similar programs are already underway at the state level.
In Clarksdale, Mississippi, the state hosted its first-ever mobile vaccinations for homebound older adults on Wednesday. That's where a bus picked up Busby outside a senior daycare and community center located next door to a low-income housing complex for the elderly.
As Busby balked, a staff member encouraged her to join the group waiting to get on board. She said later a main motivating factor for her to get the shot was the support of her brother, who called her up to encourage her to get vaccinated.
“I’m going to call him as soon as I get home, and let him know I did it,” she said, as she got back on the bus to return to the community center.
Older folks are actually less hesitant than many. According to an AP-NORC poll in late March, 11% of Americans aged 65 or older say they probably or definitely won’t get vaccinated. That compares with 25% of all adults.
The White House has repeatedly pointed to family members and community leaders as the best validators to overcome hesitance. It is also moving to create more vaccination sites closer to homes, recognizing that access concerns span demographic groups. On Wednesday, the White House announced that all of the more than 1,400 federally qualified community health centers will be able to begin administering vaccines. It also is aiming to expand mobile vaccine clinics.
A disproportionate number of unvaccinated seniors are from Black or Latino communities, or from people without easy access to health care, said Kathleen Cameron, senior director of the National Council on Aging’s Center for Healthy Aging, mirroring disparities in the broader population. And about 6% of seniors are homebound.
“Those are the hardest to reach people, and those are the ones we need to work hardest to get to, either to bring them to vaccination centers or to bring the vaccines to them,” she said.
Aurelia Jones-Taylor, CEO of Aaron E. Henry Community Health Services Center, Inc. in Clarksdale, said one of the major helps — but sometimes barriers — to getting older adults vaccinated is family members. Some encourage their relatives, helping them with rides to clinics and making sure they get their shots.
But in many cases, younger family members are misinformed about the vaccine and discourage older relatives from getting it. Aside from that, older adults can be harder to reach because they aren’t savvy on social media and live alone.
“They are stuck in the house, and they are fearful,” Jones-Taylor said. “We have to overcome the fear.”
According to the CDC, seniors, depending on their age, are between 1,300 and 8,700 times more likely to die of COVID-19 than 5-17 year-olds, and they make up more than 80% of the 559,000 U.S. fatalities due to the virus.
One major help in Mississippi – especially among older adults – is the encouragement of pastors and church communities, Jones-Taylor said.
“It’s paramount,” she said. “That’s who they listen to.”
Julia Ford, 71, spends most days at the Rev. S.L.A Jones Activity Center. She said her faith was a major motivating factor for her getting the vaccine.
“I wasn’t sure what I would do – ‘Will I get it or will I not?’ I talked to the Lord to give me understanding about it,” said Ford, whose brother died of the virus. “I thought about the verse, ‘Everything that was made was made by him.’ There was nothing made that was not made by him. He made the virus and he made the antidote.”
———
Miller reported from Washington.